22 Common Symptoms of Type II Diabetes
Friday April 13, 2018 by Marianne Gutierrez 3,606 words
1. Mood Changes
Mood change is sometimes one of the first symptoms to suggest someone may have diabetes. When there are extreme fluctuations to their mood, diabetes may be the cause. Generally the person will suddenly get impatient or angry and their friend or partner may suggest that they are hungry and need something to eat; after which the mood becomes more convivial. If this happens, it would be sensible to get checked by a GP.
Glucose is needed for the supply of energy for the nerves and the brain, it is vital. If glucose is in short supply due to a diabetic condition, the mood can vary considerably.
Studies demonstrate that depression is the problem with mood in diabetes.
Depression is common in both type 1 and type 2 diabetes and has significant effects on the course and outcome of this medical illness. Conventional antidepressant management strategies are effective and the regimen should be tailored to the individual patient. Enhanced efforts toward good glycemic control may also contribute to improvements in mood and perceptions of well-being.
VectorMine / shutterstock.com
2. Trouble Sleeping
Diabetes has a domino effect throughout the body because, as already stated, it affects the way glucose is used and glucose is essential for brain and nerve function.
The classic symptoms of uncontrolled diabetes include feeling very thirsty and having to urinate often. As a result, you may wake up several times during the night to use the bathroom and/or get something to drink … Low blood glucose, or hypoglycemia, may also wake you up during the night with symptoms of feeling sweaty, shaky, dizzy or hungry … having diabetes puts you at higher risk for sleep apnea and other sleep difficulties, such as restless legs syndrome, compared to people without diabetes. If you have sleep apnea, you may stop breathing for short periods of time while you sleep. When you stop breathing, you wake up and your breathing then returns to normal. These frequent interruptions in your sleeping pattern can prevent you from getting into deep, restful stages of sleep.
ellepigrafica / shutterstock.com
3. Excessive Thirst
If you do get checked out by a GP for diabetes, a question that will be asked is: Do you feeling thirsty all the time? Excessive thirst is caused by the kidney’s excreting more and more fluid via urine. Excess fluid is caused by excess glucose in the blood because glucose attracts water to itself which the kidneys work hard to eliminate. It is important to get checked by a GP if you suffer with excessive thirst because this causes wear and tear on the kidneys and then kidney disease could result.
Sugar is not a problem for the kidneys unless the blood sugar level gets too high. This commonly occurs in both Type 1 and Type 2 diabetes. Once the blood sugar level gets higher than 180 mg/dl, the kidneys start to spill sugar into the urine. The higher the blood sugar, the more sugar comes out in the urine. If your kidneys are normal, this usually isn’t a problem, but if you have diabetes, too much sugar can cause kidney damage.
Artie Medvedev / shutterstock.com
4. Hunger
A diet high in carbohydrates causes insulin to store the excess as fat. Too much stored fat causes another substance, leptin (a hormone produced by the body-fat that tells the brain to suppress the appetite) to be produced in excess, which then overwhelms the cells. To protect themselves against the plethora of leptin entering the cell, the cells shut down their receptors (effectively closing the leptin receptor doors of the cell) causing leptin resistance. In this case the brain doesn’t receive the message that the individual is full, and therefore continues to release hormones (messages) that signal hunger. If this reaction continues obesity and the complications of being overweight may occur.
Researchers have uncovered a destructive mechanism at the molecular level that causes a well-known phenomenon associated with obesity: leptin resistance. They found that mice fed a high-fat diet produce an enzyme named MMP-2 that clips receptors for the hormone leptin from the surface of neuronal cells in the hypothalamus. This blocks leptin from binding to its receptors. This in turn keeps the neurons from signaling that your stomach is full and you should stop eating.
Eugenio Marongiu / shutterstock.com
5. Dry Mouth
Dry mouth comes under two headings. Xerostomia is when the patient feels their mouth is dry but the measurement of salivary flow is considered to be normal, and hypo-salivation occurs when the measurement of salivary flow is lower than normal. Dry mouth can be experienced by anyone not necessarily those who have diabetes.
There are many factors that induce a dry mouth in diabetic patients from aging, radiotherapy, systemic disorders (such as chronic inflammatory disorders), medication, high intake of glucose and kidney disorders. Some cases of xerostomia are seen in patients with depression and anxiety. No review until 2016 had been presented to demonstrate whether xerostomia and hypo-salivation were more evident in diabetic patients than non diabetic patients.
The review in 2016 found only one study that hypo-salivation was higher in diabetic patients than non diabetic. But the studies researched in this review were difficult to compare due to the quality and variations; and therefore were inconsistent.
In the main it is thought that some medication used to treat diabetes can also cause a dry mouth. However high glucose intake and wear and tear on the kidneys may also play their part.
The review conducted demonstrated the considerable variation in prevalence of xerostomia and salivary flow rates among DM [diabetes mellitus] population in relation to non-DM patients. Most studies found a higher prevalence of xerostomia and lower salivary flow rates in DM with respect to CG [control group]. We found only a study about hyposalivation that showed higher prevalence in DM than non-DM patients.
Cessna152 / shutterstock.com
6. Frequent Urination
Due to the high content of glucose in the diet from refined carbohydrates, sugary foods and alcohol consumption, water is attracted from the tissues by the glucose which increases the work of the kidneys to get rid of the excess glucose and fluid and so the need to pee more.
Excessive thirst (also called polydipsia) and increased urination (also known as polyuria) are classic diabetes symptoms. When you have diabetes, excess sugar (glucose) builds up in your blood. Your kidneys are forced to work overtime to filter and absorb the excess sugar. If your kidneys can’t keep up, the excess sugar is excreted into your urine, dragging along fluids from your tissues. This triggers more frequent urination, which may leave you dehydrated. As you drink more fluids to quench your thirst, you’ll urinate even more.
kenary820 / shutterstock.com
7. Unexplained Weight Loss
Although there may be many other reasons for an unexpected loss of weight, in diabetes it is caused by insulin not getting glucose to where it is required and the body breaking down muscle tissue and fat cells to supply energy.
In all cases of unexplained weight loss, it is essential to see your Medical Practitioner.
If you have unintentionally lost more than 5% of your normal body weight, or more than 10 lbs (4.5 kg) in 6 - 12 months or less, you should consult your doctor. They will be able to determine what’s causing the weight loss (e.g. undiagnosed diabetes) and the best way to treat the problem.
Africa Studio / shutterstock.com
8. Tiredness
Those suffering with diabetes may also suffer with tiredness or fatigue but the severity of fatigue is difficult to quantify and therefore difficult to know how to treat it. Tiredness is due to interrupted sleep patterns, lack of exercise, lack of glucose for energy if insulin is not doing its work and all the other complications of diabetes. A full diagnosis of the diabetic condition will greatly help to ascertain methods to reduce tiredness.
Clinicians who work with patients affected by diabetes have noted anecdotally the considerable toll that fatigue takes on their patients, yet there is little empirical research describing the severity of the problem. Fatigue in diabetes may be associated with physiological phenomena, such as hypo- or hyperglycemia or wide swings between the two. Fatigue may also be related to psychological factors, such as depression or emotional distress related to the diagnosis or to the intensity of diabetes self-management regimens. Fatigue may also be related to such lifestyle issues as lack of physical activity or being overweight–especially common in people with type 2 diabetes. Research is needed to clarify these relationships in order to help people with diabetes manage this symptom.
file404 / shutterstock.com
9. Blurred Vision
Not everyone with diabetes suffers with blurred vision, which can be a cause of hypo-glycemia. Blurred vision may also be a symptom of diabetic retinopathy. The vision of diabetic suffers can become impaired if the disease is not managed properly. Therefore, it is important if blurred vision is experienced that you get checked out by your Doctor.
Chronically high blood sugar from diabetes is associated with damage to the tiny blood vessels in the retina, leading to diabetic retinopathy. The retina detects light and converts it to signals sent through the optic nerve to the brain. Diabetic retinopathy can cause blood vessels in the retina to leak fluid or hemorrhage (bleed), distorting vision. In its most advanced stage, new abnormal blood vessels proliferate (increase in number) on the surface of the retina, which can lead to scarring and cell loss in the retina.
kichigin / shutterstock.com
10. Headaches
Headaches are a common symptom in those with low blood sugar or hypo-glycemia. Hypo-glycemia is due to not enough glucose in the blood either because you have not eaten properly and skipped meals or because insulin is not working optimally.
The brain not receiving enough glucose causes most of the symptoms of hypoglycaemia, which include: headache, migraine, confusion, nausea, sweating, faintness, and hypothermia. If the hypoglycaemia is very severe and prolonged, it can even cause loss-of-consciousness and death, although this is rare.
Africa Studio / shutterstock.com
11. Loss of Consciousness
This is due to a hypo-glycemic condition when there is not enough glucose in the blood which the brain must have for its energy supply. It is either caused by skipping meals or because there is not enough insulin to allow glucose to get to the brain. Try consuming about 15 mgs of carbohydrate or sugar and see if there is a reduction of symptoms. If you do not feel any worse, try another 15 mgs after 15 minutes.
A low blood glucose level triggers the release of epinephrine (adrenaline), the “fight-or-flight” hormone. Epinephrine is what can cause the symptoms of hypoglycemia such as thumping heart, sweating, tingling, and anxiety. If the blood glucose level continues to drop, the brain does not get enough glucose and stops functioning as it should. This can lead to blurred vision, difficulty concentrating, confused thinking, slurred speech, numbness, and drowsiness. If blood glucose stays low for too long, starving the brain of glucose, it may lead to seizures, coma, and very rarely death.
Moriz / shutterstock.com
12. Recurrent Infections and Yeast Infections in Women
It may be time to ask your Doctor to check you for diabetes if you continually suffer with yeast infections, if the Doctor has not already discussed this with you. Yeasts need warm, moist areas to grow but also feed off sugar. A diet high in sugar would encourage yeast infections to proliferate.
Thrush is a yeast infection (candida albicans) which tends to affect warm, moist areas of the body such as the vagina, penis, mouth and certain areas of skin. Thrush is more common in people with diabetes as high sugar levels lead to better conditions for the yeast to grow. A dry mouth coupled with a higher amount of glucose in the saliva can also make for favorable conditions for thrush.
Siriluk ok / shutterstock.com
13. Slow-Healing Wounds
Nerves are damaged when the glucose they need is not available due to poor insulin supply despite the amount of glucose in the diet. In hyperglycaemia the blood glucose is too high because the body cannot utilize the glucose because not enough insulin is being made. When nerves are damaged, blood doesn’t get to the peripheries of the body and wounds are slow to heal.
Diabetic foot ulcers (DFUs), a leading cause of amputations, affect 15% of people with diabetes. A series of multiple mechanisms, including decreased cell and growth factor response, lead to diminished peripheral blood flow and decreased local angiogenesis, all of which can contribute to lack of healing in persons with DFUs.
lovelyday12 / shutterstock.com
14. Itching of the Skin in the Areas of the Groin
Itching of the skin is miserable but can be due to a yeast infection. Try using a natural product for example the essential oil of tea-tree to kill the yeast infection - mix 2 drops of tea-tree to a tea-spoon of extra virgin olive oil and apply to the itchy areas to kill the infection. Itchy skin anywhere can also be due to poor circulation in which case movement and exercise may help to increase blood to the peripheries.
Localized itching is often caused by diabetes. It can be caused by a yeast infection, dry skin, or poor circulation. When poor circulation is the cause of itching, the itchiest areas may be the lower parts of the legs. You may be able to treat itching yourself. Limit how often you bathe, particularly when the humidity is low. Use mild soap with moisturizer and apply skin cream after bathing.
Sasun Bughdaryan / shutterstock.com
15. Weight Gain
In Type 2 diabetes, the advice is to change your diet to avoid excess sugar and carbohydrate consumption and to take some exercise to reduce high blood sugar and to maintain a healthy weight. However this may not produce the hoped for results and insulin therapy may be required. When insulin therapy is working effectively, you may gain weight because not only is your body using fats and proteins properly, it is also storing the unused calories as fat. The solution is to eat smaller portion sizes.
Exercise, eat right, and stay at a healthy weight. These goals are at the core of every type 2 diabetes treatment plan. And, for some people, that’s enough. When it’s not, insulin therapy is one treatment option that can help patients, but one possible side effect is weight gain. This can become a cycle for patients who need to control both diabetes and their weight. It’s frustrating when you feel the treatment is part of the problem. With diabetes, however, you have to get the blood sugar under control first. Insulin is used because it works. The cost of insulin can vary, but lower-cost insulin is associated with more weight gain.
Odua Images / shutterstock.com
16. Dark Skin Changes of the Neck, Armpit, and Groin
These dark skin changes have a name: Acanthosis nigricans. This occurs in people who are obese or have diabetes, areas of the skin can become thickened and darkened. The cause is due to insulin resistance. Insulin resistance is when the cells refuse to respond to insulin, possibly due to not enough GLUT receptors on the cell to receive glucose. If this reaction continues Diabetes Type II will result if not already diagnosed and further complications with diabetes will ensue.
Most people who have acanthosis nigricans have also become resistant to insulin. Insulin is a hormone secreted by the pancreas that allows your body to process sugar. Insulin resistance is what eventually causes type 2 diabetes.
srisakorn wonglakorn / shutterstock.com
17. Numbness and Tingling of the Hands and Feet
Numbness and tingling of the hands and feet can be caused by other conditions not necessarily diabetes. B12 deficiency and kidney failure are also causes. In diabetes it is caused by damage to the nerves by too much or too little glucose. Nerves need glucose for their energy supply but too much damages the smaller blood vessels which reduces the nutrients the nerves need.
Diabetes can cause neuropathy as a result of high blood glucose levels damaging the small blood vessels which supply the nerves. This prevents essential nutrients reaching the nerves. The nerve fibres are then damaged or disappear.
Alice Day / shutterstock.com
18. Shaking & Sweating
Shaking and sweating is generally caused by low blood sugar when the brain, nerves and muscles are not getting the energy they need from the blood because of a lack of glucose.
All of the body’s cells need to make energy and most can use other fuels such as lipids. However, neurons (nerve cells) rely almost exclusively on glucose for their energy. This is why the maintenance of blood-glucose levels is essential for the proper functioning of the nervous system.If glucose levels fall to too low a concentration (hypoglycaemia) or rise too high (hyperglycaemia) then this situation can lead to the neurological processes in the brain being compromised. At some time, most of us will have experienced the effects of low blood glucose, a feeling of being light-headed, weak and shaky, together with an inability to concentrate properly. Chronic hyperglycaemia, which is a common feature of diabetes mellitus, also causes neurological problems and is a contributory factor to both atherosclerosis and renal failure.
Elvira Koneva / shutterstock.com
19. Sexual Dysfunction
Damage to the nerves in diabetes is caused by too much glucose damaging the smaller blood vessels which then reduces the nutrients available to the nerves. This can be caused by too high consumption of carbohydrates from foods and drinks. A lack of glucose in the blood can also damage nerves and small blood vessels because the nerves need glucose for their energy supply. Both conditions can then lead to sexual dysfunction. If this reaction continues further damage to nerves will result which may cause damage to the peripheries of the body – feet and legs.
Erectile dysfunction — the inability to get or maintain an erection firm enough for sex — is common in men who have diabetes, especially those with type 2 diabetes. It can stem from damage to nerves and blood vessels caused by poor long-term blood sugar control.
VGstockstudio / shutterstock.com
20. Family History of Diabetes
If you have a family history of diabetes, it doesn’t necessarily mean you will get the condition yourself. There are a variety of genes involved in the development of diabetes and no-one knows what triggers a gene to express itself.
Even with a set of twins which have exactly the same DNA, one may get diabetes and the other may not.
By studying identical twins, researchers from Lund University in Sweden have identified mechanisms that could be behind the development of type 2 diabetes. This may explain cases where one identical twin develops type 2 diabetes while the other remains healthy.
kenary820 / shutterstock.com
21. High Blood Pressure
High blood pressure is considered to be from 140 (Systolic) over 90 (Diastolic) and levels elevated above those numbers. Pre-high blood pressure is 120-140 over 80-90. It is the diastolic number that the Medical profession are concerned with although naturally both numbers are taken into account. Ideal blood pressure is from 90-120 over 60-80. If your blood pressure is 90⁄60 this would be low. In general terms normal blood pressure is considered to be 120⁄70. Any numbers above or below this will give your Physician cause to look at your medical history and consider your symptoms.
Why is high blood pressure involved with Type II Diabetes? While the cause of high blood pressure is unknown, it is known that other conditions play a part. Too much fluid retained causing inflammation, poor kidney filtration and elimination, medications, or lack of minerals that help reduce inflammation.
In Type II Diabetes, too much glucose in the diet causes inflammation. Sodium found in preserved meats and glucose in additives and sugar, bind to and hold on to water in the body; which is why a reduction of foods that contain the additives sodium and glucose may help reduce high blood pressure.
You probably have high blood pressure (hypertension) if your blood pressure readings are consistently 140 over 90, or higher, over a number of weeks. You may also have high blood pressure if just one of the numbers is higher than it should be over a number of weeks. If you have high blood pressure, this higher pressure puts extra strain on your heart and blood vessels.
Monkey Business Images / shutterstock.com
22. A PCOS Diagnosis
PCOS is Polycystic Ovary Syndrome which features include menstrual irregularities, sub-fertility, hyperandrogenism (excessive levels of androgens) and hirsutism (male pattern hair growth on women).
Metabolic syndrome is increased in women with PCOS.
Metabolic Syndrome is a series of metabolic disorders which include many symptoms of diabetes. Therefore, women with a diagnosis of PCOS, need to be aware of symptoms associated with diabetes and see their GP for advice as well as changing their diet.
Many patients with PCOS have features of metabolic syndrome such as visceral obesity, hyperinsulinaemia and insulin resistance. These place patients with PCOS under high risk of developing cardiovascular disease (CVD), Type 2 diabetes (DMT2) and gynecological cancer, in particular, endometrial cancer. Metabolic syndrome is also increased in infertile women with PCOS.
sirtravelalot / shutterstock.com
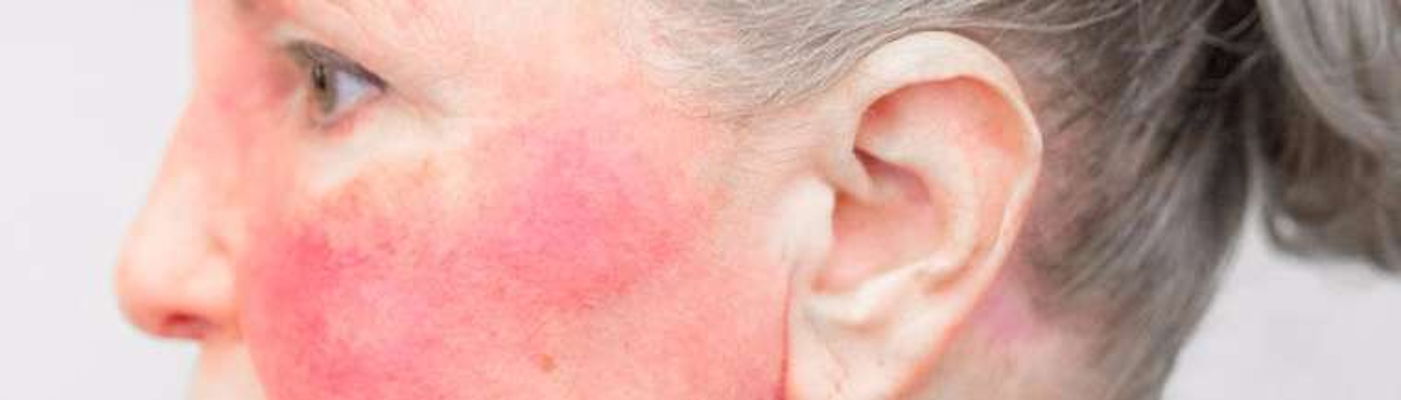
16 Warning Signs of Lupus to Watch Out For
1. Unexplained Fever Lupus can affect everyone differently and some may have …
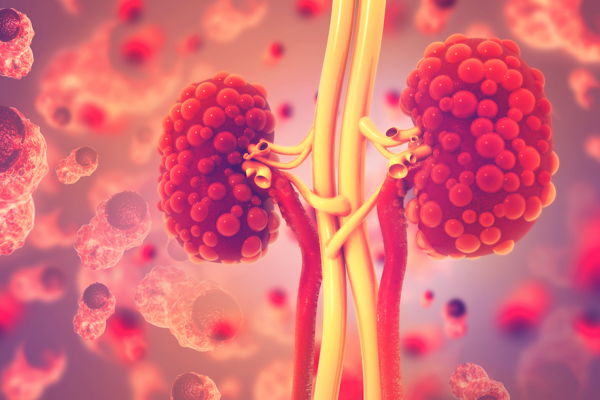
21 Features of Kidney Disease
1. Dizziness Kidney Disease is when the kidneys are not filtering blood …

Top 10 Foods to Nourish Your Thyroid
Did you know that the food you eat can affect your thyroid health? Some foods …


12 Facts About Your Borderline Personality …
1. It's Finally Classified As a Mental Illness Borderline Personality Disorder, …


12 Common Factors That Trigger Rosacea …
1. Makeup Some products used on the face and body or in the mouth ie: make-up, …


22 Common Symptoms of Type II Diabetes
1. Mood Changes Mood change is sometimes one of the first symptoms to suggest …
